If you’re just joining me here, be sure to check out Part 1 of Rhett’s birth story first here
The next two hours were a blur. The midwife on call came in, and she did her own cervical check to confirm the status. They made the decision to transfer me to a larger hospital in Portland with a NICU equipped to handle earlier premature babies than what the local hospital was capable of handling. They put magnesium into my IV, to protect and help baby’s brain develop, and at exactly 5am I received a shot of Antenatal Betamethasone, a steroid that is used to speed the baby’s lung development. You need two doses of the steroid, 24 hours apart, and then another 24 hours after the 2nd does for the steroid to be fully effective. The staff was assuring me that they would keep me pregnant for as long as possible, and I’d hopefully not deliver until 35-37 weeks along. All the while, they were making decisions showing me that was not going to happen, it wasn’t realistic based on how things were progressing.
One side effect of magnesium via IV is that it will make you hot. Really hot. I went into labor at the beginning of one of the coldest ice storms in recent Portland history. It was freezing cold and windy outside, the ambulance staff were wearing thick jackets, beanies, and gloves as they transported into the ambulance. Me? I flung off my blankets, was dripping sweat, and the cold temperature was as nice as standing in front of the AC fan on a hot August evening. I remember laboring on that plastic, skinny ambulance bed, on what felt like the longest drive of my life. My husband had gone home to take care of our dogs, throw some clothes and whatever he thought I might want for the next few days into a bag, and would meet me at the hospital. We didn’t have a hospital bag packed – I was only 32 weeks along, right?
I arrived at the new hospital around 6am, and not much happened for the next few hours—until after the shift change and the doctor discussions where they decided what to do with me. My parents had come to the hospital to be with me, and my in-laws came a little later. My contractions were still regular and intense, they had not slowed or stopped.
Around 11am, 12 hours after originally checking into the hospital, a group of 6 doctors and nurses paraded into my room. Between them, my husband, parents, and in-laws, I suddenly had 11 faces staring at me, and I was not sure why. “Emilie, we need to give you an epidural. We need you to agree to this, and to not try to be the hero. You need to rest and we think an epidural might slow down your contractions. Will you agree to this? This will be best.” I was shocked. 11 faces staring at me, half of them pressuring me, half of them just watching the scene unfold. An epidural? I hadn’t even thought that far yet. I didn’t want an epidural in my birth plan, but my birth plan is now irrelevant. I had reasons for not wanting the epidural, and not a single one applied now. I began to cry. “Okay” I said. I wasn’t sad. I was scared. Not of the epidural itself but that this was really their last and best plan? Pain relief? The doctor told me that I would need to be hospital bedrest for at least 2 weeks, and their best plan was an epidural?
By the grace of God, the epidural did help. My contractions slowed way down, they became less frequent and were at mild intensity. I did get relief from the pain. I was able to sleep, for the first time since Sunday, since I had gotten up for work Monday morning, and it was so, so good. The rest of the day and night were mild. My family eventually left and went home, or to take care of our dogs, and Josh and I were able to get some much needed rest. I was very hungry, but not allowed to eat because of the epidural regulations. One nurse snuck me some food. Thank God for those kinds of nurses. Nurses would come in and give me pills, check readings, do all of the things, and then leave us alone for the most part.
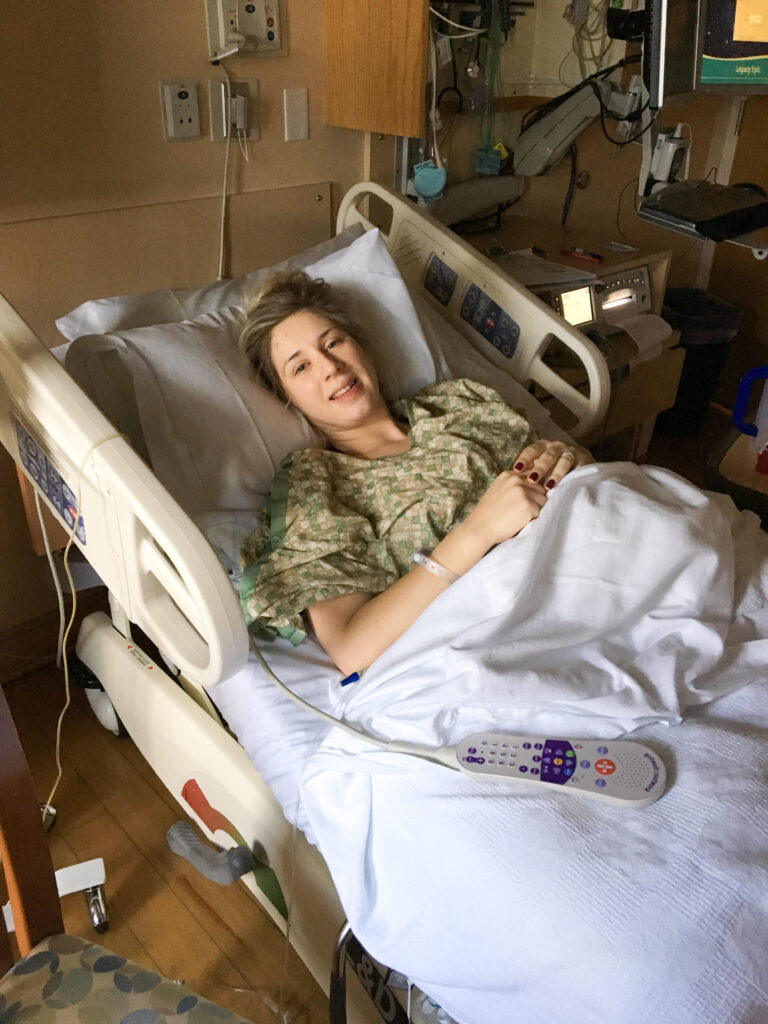
Wednesday morning, right at 5am on the dot, a nurse popped in with my 2nd steroid shot. She congratulated me on making it to my second dose. “Now you just need to hold on at least 24 more hours!” Hmm, I thought the plan was 1-2 weeks? I wondered. After the next shift change and doctor meeting, a few staff came into my room to let me know that they would be turning off my epidural. I’d still have the needle in and be hooked up, but the medication would be turned off. They wanted to see how my body was doing, if contractions were calmed down, and if my labor had progressed. I hadn’t dilated much more that last 24 hours – maybe another centimeter and slightly more effaced. My mom had come back to the hospital now to be with me.
So, off went the epidural. I was able to move around a bit, stand on the side of my bed and let the blood circulate. After 36 hours on IV fluids and lots of medications, my feet were swollen and hurting. Stepping down to the ground was like walking on needles, but I was happy to move. But then on came the contractions. Fiercely. A contraction would come, and I couldn’t talk. I became irritable. Why was my husband eating? What were they chatting about? Didn’t they see me here, in pain? The contractions hurt, but now they felt different. They were in my lower back and my hips; it scraped. My uterus contracted, but the pain was felt on my lower back. My son had flipped, causing “back labor” contractions, just in time for my epidural to be turned off. His spine was scraping against mine with every squeeze. I cried. I swore. Josh squeezed my hips during each contraction to relieve pressure. My mom held my hand. I was in agony. The nerves, the scraping, the pinching and clamping sensation. Back labor is agony. The worst pain of my life. If a normal contraction hurts, back labor is excruciating. I begged the nurse to turn my epidural back on. She asked the doctor. He said no, we needed to wait it out. I heard my nurse scold him “She is having back labor! She is hurting! Are we trying to torture her?! Please, turn it on!” An hour later (anesthesiologists are quite busy, I guess) the epidural was finally back on. This time they let me have the knob to control the medication level. I turned it way up.

It was now early afternoon, and things had calmed down. They brought in an ultrasound machine and did a series of measurements. They wanted to prep the NICU staff for his arrival—you know, just in case—and get an estimate of his stats. He was going to be about 4lbs and 18inches long. My mom decided to head back home, thinking it would be another calm night. The doctors and nurses finally left us alone, and we were able to get a few minutes of rest. Just as we were drifting to sleep…

POP. “Um, what was that?” I heard the pop on the monitors but also audibly outside of the electronics. It felt like a pressure valve was released. “Umm, did you hear that? Was that my water breaking? Excuse me, nurse?? Um, this doesn’t seem right? Josh, can you come here, is that wet under me??”
My nurse confirmed that my waters had just broken. My mom rushed back to the hospital. The doctor said just to wait and she’d come back in a while to check on me. She waited a long time, a few hours. They wanted me to “labor down” which basically means not encouraging any pushing until mom feels like she absolutely cannot not push. I was thankful for this, although it felt like a year, I was so, so tired and was okay waiting. Praise the Lord that my baby flipped back over into the correct position, and contractions were back to normal pains. I still had the epidural on, but still felt every contraction. I had not truly slept in days, and hadn’t eaten hardly anything. The last few days had been an emotional rollercoaster. It was now really go-time, I was about to meet my child, and yet I had no energy.
The exhaustion finally caught up with me and I just couldn’t. I tried. I tried to push and push. I had no more to give. With each contraction and push, heartburn ripped up my throat. I thought I would vomit, each squeeze and strain more severe. I strained, but I wasn’t getting far. I couldn’t. He was moving down, but I could not help him. My body had nothing else to offer. My contractions went from every minute, to every few minutes, to basically stopping. I was trying but my body was done. But we were too far. He was determined to come out and was fully in the birthing canal, and at risk of being stuck. I was put on an oxygen mask and given Pitocin in my IV to stimulate my contractions.
With the help of the oxygen and Pitocin, I had energy for a few more pushes. “I can see his head! Do you want to reach down and feel your son’s head? He has thick dark hair!” I cried. I reached down. It was so strange. That was the first time I got to touch my baby, and wouldn’t again for several hours. His heart rate was starting to drop, he’d been in there too long. Even I could hear his heartbeat slow on the monitor. My doctor yelled at me, “You HAVE to do this! I need a big strong push!” With tears in my eyes, I gave it my all, one last strong push his head crowned just enough for the doctor to reach her hand deeply and around his head and pull him out. On Wednesday, December 7th, at 8:14pm, at 32 weeks and 3 days gestation, my son was born. After 3 ½ days of labor, my son was here.
He wasn’t placed on my chest. The doctor held him at my legs, lower than my body, so that all of the blood would effortlessly drain down into his body, not allowing his little heart to work too hard to pump blood against gravity. Josh was able to cut the cord about a minute later, and my sweet boy was taken off to the Neonatal Intensive Care Unit (NICU). My labor and delivery were officially, finally over.
Rhett was born weighing (a swollen) 5lbs, 4oz, and was 18 inches long. He spent the next 23 days and nights in the NICU, learning to breathe, swallow, grow, and get stronger. But that story is a story for another time!

+ COMMENTS
add a comment